19 Apr 2026
- 0 Comments
Imagine reaching for a white oval pill, thinking it's your blood pressure medication, only to realize later it was actually a sleeping pill. For millions of people, this isn't a hypothetical scenario-it's a daily risk. When you can't clearly read a label or hear a pharmacist's instructions over the noise of a busy store, taking the right dose of the right medicine becomes a gamble. Whether it's due to age-related macular degeneration or profound hearing loss, sensory impairments create a dangerous gap in healthcare that often goes unnoticed by the professionals providing the care.
The reality is stark: people with visual impairments are nearly 1.7 times more likely to make medication errors than those with full sight. From missing an expiration date to confusing two similar-looking bottles, these mistakes aren't about a lack of care; they're about a system designed for people who can see 7-point font. But you don't have to rely on luck. By using a mix of low-tech hacks and modern tools, you can take control of your medication safety and stop the guesswork.
The Real-World Challenges of Sensory Impairment
For many, the struggle starts at the pharmacy counter. Standard prescription labels use tiny fonts that are virtually invisible to someone with low vision. Even when the text is legible, glare from glossy paper or tape can make reading impossible. Then there's the auditory side: pharmacy environments are often loud, making it hard for those with hearing loss to catch critical dosing warnings or side-effect cautions during a quick consultation.
Not all medications are created equal when it comes to difficulty. While tablets and capsules are generally easier to manage, liquid medications and eye or ear drops are significantly more challenging. Why? Because they require precise measurements and steady visual coordination to ensure the dose is correct. Without a way to verify the level of a liquid in a clear bottle, the risk of under-dosing or over-dosing spikes.
Beyond the pharmacy, there is a systemic failure in packaging. While some boxes include Braille, it's often limited to the name of the drug. Crucial information, like how many times a day to take the pill, is rarely included in Braille, leaving users dependent on others or risky guesswork.
Low-Tech Hacks for Immediate Safety
You don't need expensive gadgets to make your medicine cabinet safer. Some of the most effective solutions are the simplest ones that you can implement today. The goal is to create a physical "code" that doesn't rely on sight or sound.
- Tactile Markers: Use rubber bands to indicate frequency. For example, one rubber band around the bottle for once-a-day meds and two for twice-a-day meds.
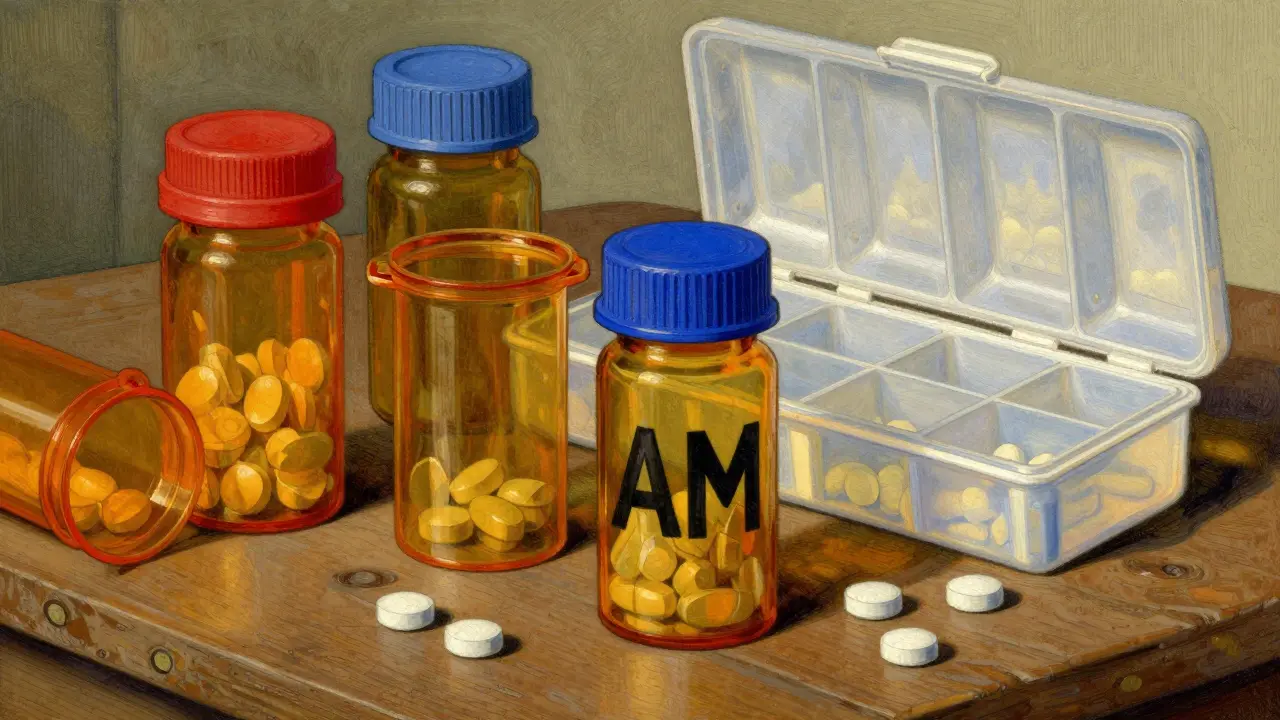
- High-Contrast Labeling: Use a thick black permanent marker to write "AM" or "PM" in large letters on the side of the bottle.
- Color Coding: Assign a color to each time of day. A red sticker or cap for morning meds and a blue one for night. This is one of the fastest systems to learn and implement.
- Physical Organization: Use a pill organizer with oversized compartments. Arrange them logically-left to right for the day, top to bottom for the time.
| Solution | Effectiveness | Learning Curve | Primary Drawback |
|---|---|---|---|
| Color Coding | ~78% | Short (1.2 weeks) | Useless for total blindness |
| Rubber Bands | ~65% | Very Short | Inconsistent interpretation |
| Braille Labels | ~85% | Long (requires literacy) | Low adult literacy rates |
| Talking Rx Devices | ~92% | Medium (4.3 weeks) | Higher cost |
Leveraging Technology and Professional Support
When low-tech options aren't enough, technology can bridge the gap. For those who struggle with reading, Talking Rx devices allow a pharmacist to record up to 60 seconds of verbal instructions that the patient can play back at home. This removes the stress of remembering a conversation held in a noisy pharmacy.
Digital tools are also evolving. Apps that use the camera to read labels aloud or voice-activated medication reminders are becoming more common. To be truly effective, these tools should follow WCAG 2.1 AA accessibility standards, ensuring they work seamlessly with screen readers and voice commands.
However, the most powerful tool is a proactive relationship with your pharmacist. Don't be afraid to ask for specific accommodations. According to the American Foundation for the Blind (AFB), pharmacists should ideally spend an extra 3-5 minutes with visually impaired patients to ensure labels are correct and counseling is understood. If your current pharmacy isn't willing to do this, it may be time to find one that prioritizes accessibility.
How to Advocate for Your Safety
Many people feel embarrassed to tell their doctor or pharmacist that they can't read the label. This creates a "dangerous feedback loop" where the provider thinks everything is fine, while the patient is struggling in secret. Breaking this silence is the first step toward safety.
When you visit your healthcare provider, be specific about what you need. Instead of saying "I have trouble seeing," try these concrete requests:
- "Please print my labels in 18-point font or larger."
- "Can you provide a written summary of the dosage in a high-contrast format?"
- "I need a pharmacist to walk me through these medications slowly and clearly, away from the noise of the main counter."
- "Can we use a pill-packaging system, like blister cards, that helps me track if I've taken my dose?"
If you are dealing with polypharmacy-taking five or more medications daily-the risk of error grows exponentially. In these cases, ask your doctor for a "medication review." This is a dedicated session to simplify your regimen, remove unnecessary drugs, and ensure that the timing of each dose is optimized for your routine.

Common Pitfalls to Avoid
Even with a system in place, a few common mistakes can undermine your safety. One major risk is the "generic switch." Pharmacies often switch a brand-name drug for a generic version to save costs. While the medicine is the same, the pill's color, shape, and size often change. If you rely on visual identification, a generic switch can be catastrophic. Always ask your pharmacist to alert you if the physical appearance of your medication changes.
Another pitfall is relying solely on memory or a single method of identification. For example, if you only use color coding, a power outage or poor lighting can make those colors look the same. The safest approach is "redundancy"-using two or more methods. Pair a color-coded cap with a tactile rubber band. This way, if one fails, the other still protects you.
What is the best way to identify medications if I can't see the labels?
The most effective approach is redundancy. Combine tactile markers (like rubber bands for frequency) with high-contrast visual cues (like large AM/PM lettering). For those with higher needs, Talking Rx devices or pharmacy-provided Braille labels are highly effective, though the latter requires Braille literacy.
How can I ensure I don't take expired medication?
Since expiration dates are usually printed in tiny font, ask your pharmacist to mark the expiration date using a tactile sticker or a large-print label. Alternatively, use a digital medication management app that sends alerts when a prescription is nearing its end date.
What should I do if my pharmacist refuses to provide accessible labels?
Remind them that reasonable accommodations are a matter of patient safety. You can reference the American Foundation for the Blind (AFB) guidelines, which suggest 18-point font for low-vision patients. If the pharmacy cannot meet these needs, consider switching to a provider that specializes in accessible healthcare.
Are liquid medications riskier than tablets for people with low vision?
Yes, liquid medications generally have lower success rates in administration because they require measuring volumes in a cup or syringe. To mitigate this, use oral syringes with high-contrast markings or ask for pre-measured unit-dose packaging if available.
How do I handle hearing loss during a pharmacy consultation?
Ask the pharmacist to move to a quieter area of the store to reduce background noise. If you use a hearing aid, ensure it is properly adjusted, and don't hesitate to ask the pharmacist to write down key instructions or use a digital communication app on a tablet or phone.
Next Steps for Your Safety Journey
If you're feeling overwhelmed, start with one small change this week. Pick your most critical medication-the one you absolutely cannot miss or double-dose-and apply a high-contrast marker or a rubber band to it today. Once that feels comfortable, move on to the rest of your cabinet.
For those managing complex schedules, your next step should be a consultation with an Occupational Therapist. They specialize in environmental modifications and can help you set up a "medication station" in your home that uses contrast enhancement and lighting to make your routine foolproof. Remember, this isn't about convenience; it's about your health and independence.

